|
However, antibodies against MOG and their role in CNS demyelinating diseases were still of interest, and a breakthrough succeeded with the development of assay-detecting antibodies against conformational MOG. These assays recognized MOG lacking the correct membrane topology and glycosylation ( 32). coli using different test mechanisms, such as enzyme-linked immunosorbent assay (ELISA) or western blot. One problem was that many of the initial studies analyzed antibodies against recombinant linear or refolded human MOG expressed in E. Numerous studies addressed the diagnostic, prognostic, and pathogenic relevance of MOG antibodies in multiple sclerosis and other CNS demyelinating diseases with controversial results. Monoclonal MOG antibodies can cause demyelination in the presence of complement, can induce relapses, and are crucial for myelin phagocytosis of macrophages ( 32).Īlthough the role of MOG is well established in animal models, its relevance in human diseases was less clear. Furthermore, in animal models, antibodies against MOG can enhance demyelination and inflammation. It is well-known that in experimental autoimmune encephalomyelitis, MOG is a dominant antigen structure after immunization with CNS tissue homogenates ( 25). The exact biological role of MOG remains unclear. MOG, a protein of 245 amino acids, exposed an immunoglobulin domain in the extracellular space and, therefore, seems to be a potential target structure for an autoimmune reaction against myelin. The most promising results came from studies using cell-based assays expressing full-length, conformationally correct folded myelin oligodendrocyte glycoprotein, which is a protein exclusively present in the CNS at the outermost surface of myelin sheaths and oligodendrocyte membranes. Numerous potential antigen targets were studied. However, there is still a lack of biological markers for the identification of multiple sclerosis subtypes, AQP-4-negative neuromyelitis optica spectrum disorder cases, ADEM, and other atypical CNS demyelinating diseases. Knowledge of immunopathogenesis and the diagnostic management changed, and now antibodies against AQP-4 are well integrated in the clinical diagnostic procedures. A breakthrough was the detection of aquaporin-4 (AQP-4) antibodies in neuromyelitis optica spectrum disorder ( 26). Due to diagnostic role of autoantibodies in other autoimmune diseases and evidence for crucial involvement of B cells and antibodies in multiple sclerosis pathogenesis, an international research focus has been directed to antibodies against CNS antigens. In inflammatory demyelinating CNS diseases, it is suggested that an autoimmune reaction finally leading to the cascade of inflammation, demyelination, and axonal loss initiates the development of the disease. Therefore, there is a need for reliable biological markers for diagnostic and prognostic purposes. Despite typical clinical features and paraclinical markers (MRI and cerebrospinal fluid), diagnosis is often challenging. As early treatment initiation is recommended in multiple sclerosis, diagnosis at disease onset is important for patient management and treatment stratification. MOG antibodies are associated with a distinct neuropathology.Īpart from multiple sclerosis as the most common inflammatory demyelinating central nervous system disease, other rare entities, such as neuromyelitis optica spectrum diseases or ADEM, must be considered as differential diagnosis in patients with a first demyelinating event. 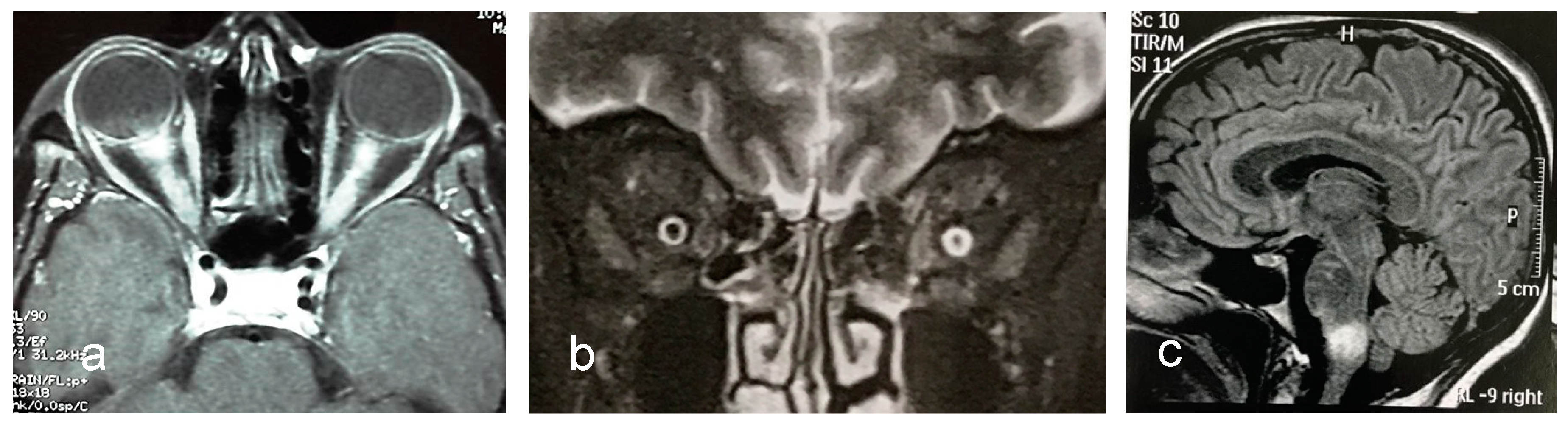
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
